 Pulmonary manifestations, such as wheezing and shortness of breathīladder or bowel incontinence (due to spinal cord lesions) Symptoms of DCS (listed in decreasing order of overall prevalence): The onset of symptoms within 10 minutes is more suggestive of gas embolism, whereas DCS tends to present after 10 minutes. The median time to symptom/sign onset is 30 minutes and severe neurologic symptoms tend to present within 10 minutes.ĩ0% of patients will experience onset of some symptoms or signs within 3 hours, and nearly all experience symptoms or signs within 24 hours of emerging from the water. 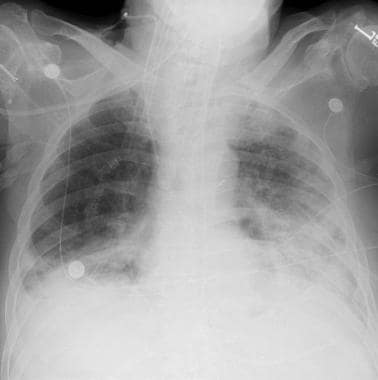
Time of onset and the specific symptoms/signs aid in establishing the diagnosis. Sinuses: Sinus pressure and pain may be observed in divers who dive with sinus congestion or when the effect of decongestants wears off during diving.Īre you sure your patient has decompression syndrome or barotrauma? What should you expect to find?ĭecompression syndrome is a clinical diagnosis. 
Symptoms of vertigo may be related to rupture of the round window or, in the acute setting, may reflect neurologic involvement of DCS. Otherwise, pain followed by hemorrhage, development of serous middle ear effusion, or tympanic membrane rupture may develop. Auto-insufflation involves forcing air up the Eustachian tube, typically by swallowing or by performing a Valsalva maneuver. As surrounding water pressure increases, a diver must be able to equalize the pressure in the middle ear by auto-insufflation. Middle ear: Injury is commonly seen in inexperienced divers who are not adept at equalizing middle ear pressures during descent. Holding one’s breath or performing a Valsalva maneuver during ascent may result in pulmonary barotrauma. The doctor will also consider any risk of recurrence of the condition that required the thoracotomy, any other medical conditions you might have, your overall level of fitness and your smoking history, all of which are necessary to consider before you return to diving.Lungs: Injury arises from pulmonary overinflation due to decreasing surrounding atmospheric pressure during ascent (as described by Boyle’s law). A follow-up appointment with a pulmonologist after the CT scan is necessary to exclude air trapping and adhesions before diving. Understanding the possible dangers and emphasising the importance of a slow ascent rate while diving may reduce this risk.Ī high-resolution spiral lung CT scan may show the extent of scarring, adhesions and the presence of any air trapping. When barotrauma occurs, air can escape from the injured lung and enter other areas of the chest, causing a life-threatening emergency.Įscaped gas from the lungs can enter one of three places: the mediastinal area around the heart (causing pneumo-mediastinum or mediastinal emphysema), the pleural space between the lung and the chest wall (causing pneumothorax), and the bloodstream (causing arterial gas embolism). Pulmonary barotrauma usually happens near the end of a dive when a diver is ascending and trapped air in the lungs is expanding due to the decrease in pressure. 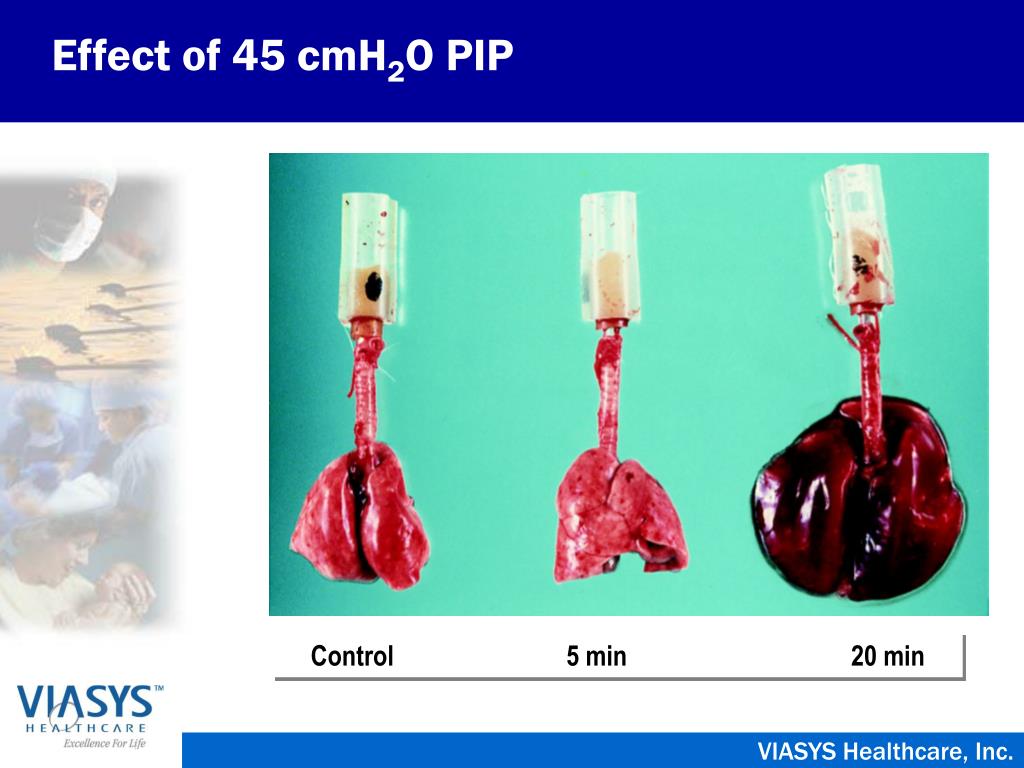
Any weakness in lung structure may be prone to rupture from even minimal over-inflation. 
Fibrotic or scarred tissue is of concern to scuba divers because it has reduced elasticity and compliance in its interface with normal lung tissue. Since barotrauma can occur with hyperinflation of lung tissue, a diver’s lungs must be able to tolerate rapid changes in volume and pressure. Is it safe to dive after this condition, or is there too much risk?Ī: The main points to consider are the risk of pleural adhesions and pulmonary scar tissue caused by the thoracotomy, which can predispose you to pulmonary barotrauma. I had pneumonia in 2015 and as a result had lung surgery (thoracotomy) to drain an empyema. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
